Researchers have discovered how psoriasis can develop into a joint disease in some patients without them noticing. Immune cells formed in the inflamed skin can enter the joints via the bloodstream, where they sometimes trigger inflammation. The key difference lies in the joint’s ability to keep these cells in check. This finding could help doctors recognize warning signs early on and prevent permanent joint damage.
What is Psoriasis?
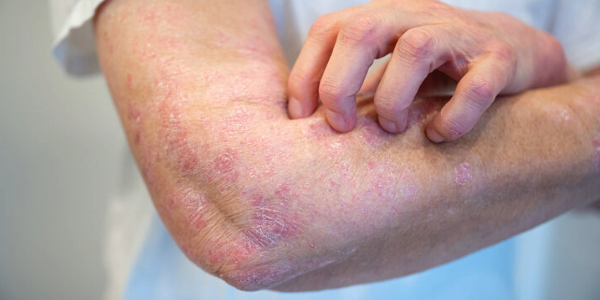
Psoriasis is a chronic, noncontagious skin condition in which skin cells renew themselves much faster than normal. This leads to characteristic skin changes: red, sharply defined patches that are often covered with silvery-white scales. These so-called plaques occur particularly frequently on the elbows, knees, scalp, or lower back, but can essentially develop anywhere on the body.
Psoriasis is caused by an abnormal immune system response. In this process, certain immune cells mistakenly attack the body’s own skin cells, leading to inflammation and accelerated cell division. The exact cause is complex and is influenced by a combination of genetic predisposition and external factors. Such triggers include, for example, stress, infections, skin injuries, or certain medications.
In addition to visible skin changes, psoriasis can also be associated with itching, burning, or pain. In some cases, the joints are also affected; this is referred to as psoriatic arthritis. About 20 to 30 percent of people with psoriasis eventually develop painful joint inflammation. This condition, known as psoriatic arthritis, can lead to permanent damage to bones and joints if left untreated. For years, it was not entirely clear to doctors why psoriasis progressed to a joint disease in some patients but not in others.
A complete cure is not currently possible, but there are many treatment options that can significantly alleviate symptoms and improve quality of life. These include topical creams and ointments, light therapy, and, in more severe cases, medications that affect the immune system.
How Immune Cells Tavel from the Skin to the Joints
Researchers from the Department of Internal Medicine 3 – Rheumatology and Immunology at the University Hospital Erlangen of Friedrich-Alexander University Erlangen-Nuremberg (FAU) have now identified the specific immune cells responsible for this and uncovered how they migrate from the skin to the joints. Their findings point to new ways to detect and prevent psoriatic arthritis before permanent joint damage occurs. The study was published in Nature Immunology.
Psoriasis causes inflammation in the skin, leading to the formation of specific immune precursor cells. These cells are not confined to the skin. According to the researchers, they can enter the bloodstream and later reach the joints. “These cells can migrate from the skin into the bloodstream and from there to the joints,” explains Dr. Simon Rauber, head of the research group at the Institute of Internal Medicine 3. He notes, however, that their mere presence does not automatically cause joint inflammation. “It is interesting that the mere migration of immune cells into the joint is not sufficient to trigger inflammation there.”
Why Joint Inflammation Develops in Some Patients
What happens within the joint itself plays a crucial role. Once immune cells arrive there, they interact with fibroblasts—connective tissue cells that normally help maintain balance and protect the joint. In people who later develop psoriatic arthritis, this protective response is weakened.” “The protective function of these connective tissue cells is generally significantly impaired in people who develop psoriatic arthritis,” said Prof. Dr. Andreas Ramming, team leader and deputy head of the Department of Internal Medicine 3. “As a result, the inflammatory cells invading the joint cannot be kept in check and trigger an inflammatory reaction in the joint.” This breakdown helps explain why some psoriasis patients develop joint disease while others do not.
The researchers also found that these migrating immune cells can already be detected in the blood before joint inflammation sets in. This discovery could make it possible to identify patients at increased risk earlier than ever before. In the future, treatments could focus on combating these immune cells before they reach the joints, thereby stopping inflammation before it begins. Such approaches could help prevent psoriatic arthritis rather than treating damage that has already occurred.