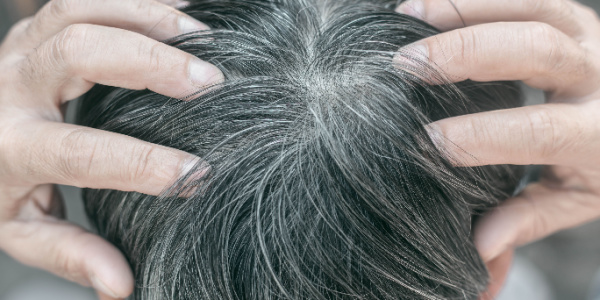
As we age, our appearance changes more and more. One sign of the aging process that many of us would like to reverse is graying hair. But how does it occur? In fact, certain stem cells have the unique ability to move between growth compartments in hair follicles, but get stuck with age, thus losing their ability to mature and maintain hair color. This shows a new study.
The Role of Melanocyte Stem Cells in the Development of Gray Hair
Led by researchers from NYU Grossman School of Medicine, the work focused on cells in the skin of mice that have also been found in humans, called melanocyte stem cells, or McSCs. Hair color is controlled by whether nonfunctional but continuously proliferating pools of McSCs within hair follicles are signaled to become mature cells that produce the protein pigments responsible for color. The new study, published online in the journal Nature, shows that McSCs are remarkably plastic. This means that during normal hair growth, such cells continuously move back and forth along the maturation axis as they switch back and forth between compartments of the developing hair follicle. In these compartments, McSCs are exposed to different levels of maturation-influencing protein signals.
Specifically, the research team found that McSCs change between their most primitive stem cell state and the next phase of their maturation, the transit-amplifying state, and depending on their location. The researchers found that as hair ages, falls out and then regrows repeatedly, an increasing number of McSCs get stuck in the stem cell compartment called the hair follicle ridge. There they stay, do not mature into the transit-amplifying state, and do not migrate back to their original location in the germinal compartment where WNT proteins would have nudged them into pigment cells for regeneration. The newly discovered mechanisms raise the possibility that the same fixed positioning of melanocyte stem cells could exist in humans. If so, it presents a potential way to reverse or prevent human hair graying by helping trapped cells to move back between developing hair follicles.
Reverse Gray Hair
Researchers say McSC plasticity is absent in other self-regenerating stem cells, such as those that make up the hair follicles themselves, which are known to move in only one direction along a fixed time axis during their maturation. For example, transit-amplifying hair follicle cells never revert to their original stem cell state. This partially explains why hair can continue to grow even when its pigmentation fails. Previous work by the same research team at NYU showed that WNT signaling was required to stimulate McSCs to mature and produce pigment. This study had also shown that McSCs in the hair follicle ridge were exposed to WNT signals many trillions of times less than in the hair germ compartment, which is located just below the ridge.
In the most recent experiments on mice whose hair was physically aged through plucking and forced regrowth, the number of hair follicles with McSCs in the follicular dome increased from 15 percent before plucking to almost half after forced aging. These cells remained unable to regenerate or mature into pigment-producing melanocytes. The researchers found that the stuck McSCs ceased their regenerative behavior as they were no longer exposed to much WNT signaling, and hence their ability to produce pigment in new hair follicles, which continued to grow.
In contrast, other McSCs that moved back and forth between the follicle ridge and hair germ retained their ability to regenerate as McSCs, mature into melanocytes, and produce pigment throughout the two-year study period. It is the loss of the chameleon -like function in melanocyte stem cells that may be responsible for graying and hair color loss. These results suggest that melanocyte stem cell motility and reversible differentiation are key to keeping hair healthy and full of color.
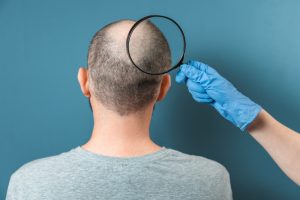
How the Immune System Causes Hair Loss
There are different forms of alopecia. Androgenetic alopecia becomes more common with age. More than 70 percent of men and almost 60 percent of all women over 80 are affected. Scientists have discovered an unexpected molecular target of a common treatment for alopecia, a condition in which a person’s immune system attacks their own hair follicles and triggers hair loss. The research describes how immune cells called regulatory T cells interact with skin cells by using a hormone as a messenger to create new hair follicles and hair growth. Salk scientists have discovered an unexpected molecular target of a common treatment for alopecia, a condition in which a person’s immune system attacks their own hair follicles and causes hair loss. The findings, published in Nature Immunology, describe how immune cells called regulatory T cells interact with skin cells by using a hormone as a messenger to create new hair follicles and hair growth.
Regulatory T cells have long been studied for reducing excessive immune responses in autoimmune diseases. The scientists were able to identify the upstream hormonal signal and downstream growth factor that actually promote hair growth and regeneration, completely independent of suppressing the immune response.
Scientists didn’t begin by studying hair loss. They were interested in exploring the role of regulatory T cells and glucocorticoid hormones in autoimmune diseases. They first investigated how these immune components function in multiple sclerosis, Crohn’s disease and asthma. They found that glucocorticoids and regulatory T cells did not work together to play a significant role in these diseases. They thought they would have more success if they looked at environments where regulatory T cells express particularly high levels of glucocorticoid receptors, such as B. in skin tissue.
Regulatory T Cells and Hair Follicle Stem Cells Promote Hair Regeneration
The scientists induced hair loss in normal mice and mice lacking glucocorticoid receptors in their regulatory T cells. After two weeks, they saw a noticeable difference between the mice – the normal mice were growing hair back, but the mice without glucocorticoid receptors hardly did. The results suggest that some form of communication between regulatory T cells and hair follicle stem cells must take place to enable hair regeneration. The scientists then used different techniques to monitor multicellular communication to study how the regulatory T cells and glucocorticoid receptors behave in skin tissue samples. They found that glucocorticoids instruct regulatory T cells to activate hair follicle stem cells, leading to hair growth.
This crosstalk between the T cells and the stem cells depends on a mechanism whereby glucocorticoid receptors induce the production of the protein TGF-beta3, all within the regulatory T cells. TGF-beta3 then activates the hair follicle stem cells to differentiate into new hair follicles, promoting hair growth. Additional analyzes confirmed that this signaling pathway was completely independent of the ability of regulatory T cells to keep the immune system in balance. However, regulatory T cells do not normally produce TGF-beta3 as they did here. When the scientists searched databases, they found that this phenomenon occurs in injured muscle and heart tissue, similar to how hair removal in this study simulated injury to skin tissue.
In acute cases of alopecia, immune cells attack skin tissue and cause hair loss. The usual remedy is to use glucocorticoids to block the immune response in the skin from attacking the hair follicles further. Glucocorticoid use has the dual benefit of stimulating the regulatory T cells in the skin to produce TGF-beta3, thereby stimulating the activation of hair follicle stem cells. This study shows that regulatory T cells and glucocorticoid hormones are not only immunosuppressants but also have a regenerative function.