Most women have experienced a change in their bladder function as they age, but for many, few understand the reasons behind this change. At some point during women’s reproductive years, women may experience an overactive bladder as the body undergoes changes that occur with menopause. Understanding what’s happening is key to managing the irritation and possible discomfort that accompanies this condition.
What Causes Overactive Bladder?
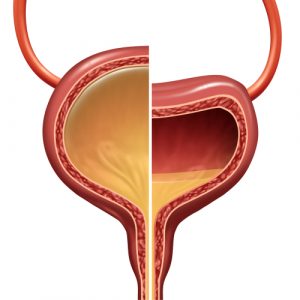
The bladder is a hollow, muscular organ that expands and contracts to store urine. It has two sphincter muscles (the urethral and the pelvic) that control the release of urine from the bladder. In women, these muscles become weak or paralyzed during menopause, causing an overactive urinary bladder. Also, as a result of hormonal changes, the bladder muscles lose their tone and become flaccid (relaxed and floppy). This combination of weak muscle tone and overactive urinary bladder causes the involuntary loss of urine.
When these changes occur, the nerves in your bladder become more sensitive to stimulation. Such stimulation may be caused by changes in the amount of urine in the bladder (a full or empty bladder), some medications, or other steps you can take to manage your overactive urinary bladder.
The Link Between Perimenopause and an Overactive Bladder
Perimenopause is when a woman going through the menopause stages experiences many changes in her body. Between perimenopause and post menopause, a woman’s body undergoes physical changes that affect several parts of her life. Perimenopause can last from three to five years and can be defined as a transitional period between menopause and post menopause. In perimenopause, a woman may experience hot flashes, night sweats, vaginal dryness, or recurrent urinary tract infections.
In this transitional period between menopause and post menopause, many women have to deal with an overactive urinary bladder or urge incontinence. The change in how hormones work during perimenopause can cause some women to feel pressure and pain in their bladder when standing up after sitting or while walking. This discomfort can make daily activities difficult, if not impossible.
Symptoms of Overactive Bladder (OAB)
- Pressure or pain in the bladder
- Feeling the need to urinate more often than usual (urge incontinence)
- Feeling the need to rush to the toilet
- Urinating small amounts at frequent intervals
- Feeling like you have to urinate but are unable to pass any urine (urinary retention)
Before diagnosing an OAB, your doctor may conduct several tests if you present some. These tests may include:
- A history of the symptoms and how often they occur
- A physical examination of your bladder and pelvic region, including a pelvic exam
- Possible testing of your urine for bacteria or other causes of infection
- Possible imaging tests, such as ultrasound or magnetic.
Menopause and an OAB
The menopause stage is the time of life when a woman stops having menstrual periods. During this period, a woman’s vagina loses its ability to contract naturally (that is to say, without medication). This process often starts about two years before menopause. In addition to the natural changes a woman goes through during perimenopause (for instance, an OAB), some women find that their bladder becomes less “relaxed” after going through menopause. A woman’s age may cause this change.
A woman between 50 and 54 years-old experiences more difficulties with an OAB than a woman from ages 55 to 59, who will have more difficulties than a woman of 60 years or older. In addition, some symptoms associated with an OAB can worsen as women get older. For instance, when women are younger than 60 years, continent urinary incontinence is the most common form of urinary incontinence. But, when women are older than 60 years old, urge incontinence is the most common form of urinary incontinence.
Dealing with an OAB During Menopause
Here are some tips that may help you control your overactive bladder:
1. Drink plenty of fluids
Water will help keep your urine from getting too concentrated and causing an OAB or urge incontinence. A general rule is to drink at least one glass of water before going to the bathroom. Women who experience an overactive bladder should drink two glasses of water daily.
2. Eat a healthy diet rich in fruits and vegetables
For some women, the need for more fluids may result from low levels of protein in their diet (which may cause the bladder muscles to become weaker), so eating healthy foods rich in protein will help prevent this occurrence.
3. Take a multimineral supplement
Taking a multimineral supplement can be effective in helping reduce urinary frequency, urgency, and incontinence in perimenopausal women. Multi minerals will help strengthen your bladder muscles and help you combat the effects of these changes in your body more effectively. Take one bottle of the liquid multimineral supplement daily (most contain calcium, magnesium, and vitamin B6), mixed into a glass of water or juice after meals.
4. Maintain a healthy lifestyle
A healthy lifestyle includes eating healthy foods, losing excess weight, getting enough sleep, and exercising regularly. These strategies will help by reducing the risk of an overactive bladder.
5. Take care of your pelvic floor muscles
Urethral hypertonicity is mild incontinence caused by changes in pelvic floor muscles that weakens these muscles, leading to an overactive bladder and urge incontinence.
For a detailed look at how to Work Your Pelvic Floor to Overcome Urinary Incontinence, click here.
OAB is a fairly common disorder and can cause many problems. Women who have it should look for solutions to their symptoms as soon as possible so that they don’t have to go through surgeries to fix the problem. Eating healthy food, drinking plenty of water, practicing good bladder habits such as frequent urination, and avoiding constipation can help make the symptoms of an overactive bladder less severe.





