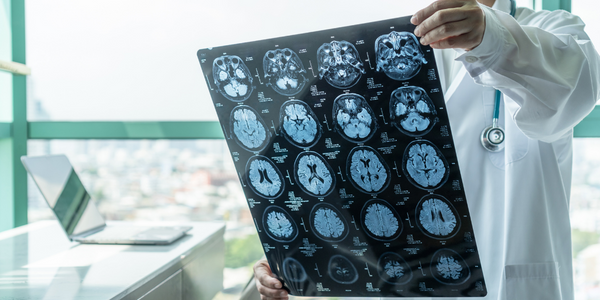
Alzheimer’s disease, the most common form of dementia in the elderly, impairs cognitive ability. That being said, research is illustrating how sophisticated imaging can reveal how the disease kills brain synapses, providing more knowledge about the disease that can be used with diagnosis, treatment and prevention.
More About the Disease
One in eight people over the age of 65 has Alzheimer’s disease in the USA. By 2050, it is estimated that 82 million people worldwide are predicted to have the condition to some extent. The signs and symptoms of the disease appear progressively over a long time and then worsen as multiple brain functions are impacted. In most cases, mild memory issues are the initial indication of the disease. The memory issues get more severe as the illness worsens, and other symptoms, such as confusion, speech difficulties, anxiety, and hallucination, appear later.
Plaques and protein clumps accumulate in the brain as the symptoms of the disease deteriorate with time. The protein and plaques ultimately lead to the destruction of synapses, which link nerve cells. According to researchers, the persistent nature of the disease’s symptoms is caused by this decline in synapse density.
Advanced Imaging Research on Alzheimer’s Disease
In recent years, advanced imaging has become a vital tool for determining which brain parts are impacted by dementia. These methods help doctors identify Mild Cognitive Impairment (MCI) caused by Alzheimer’s disease and other dementia-causing syndromes while the individual is still alive. Three distinct detection methods are now offering excellent promise for detecting the disease. They include magnetic resonance imaging, computerized tomography, and positron emission tomography.
According to a study released in the journal “Alzheimer’s & Dementia,” researchers from Yale University have confirmed that the degeneration of brain synapses causes the brain abnormalities felt by patients with the illness.

The use of PET scanning tests is done to determine glucose metabolism, this is because 95 percent of the brain’s energy originates from glucose metabolism.
In Alzheimer’s disease, the parietal and temporal lobes take in less glucose during rest. This shift in glucose metabolism coincides with senile plaque volume.
Higher cerebral blood flow is needed to deliver glucose to meet increased metabolic needs because neurons can’t store it. In dementing illnesses, diminished glucose transport and neuronal density cause impaired glucose metabolism. Therefore, the reduction in cerebral metabolism involves not only a decreased glucose metabolism from a lower tissue density but also a loss of synapses.
In the study, scientists from the Yale University Alzheimer’s Disease Research Centre, led by Dr. Adam Mecca, examined 45 individuals between 50 and 85. Cognitive tests were tested, including language skills, processing speed, visual-spatial ability, verbal memory, and executive function. After tests were given, the patients underwent imaging done by the PET scanning machine. Amazing results showed that plaque build-up in the brain meant that the subjects had the disease in its early stages.
Performance was predicted by synapse density across all assessed major domains of cognition, and the test results were lower in those with lesser synaptic density. During the study, researchers also considered the general decrease in brain volume that might happen as the disease worsens, and they realized that the link remained consistent. Moreover, the relationship between reduced synapse density and declining cognition persisted even when the researchers considered the subjects’ ages, sexes, and education levels.
They discovered that poor performance on psychological ability was closely related to the loss of synapses. Additionally, they found that the loss of synapses was a better predictor of poor cognitive function than the reduction in the total number of the brain’s neurons.
Gray matter volume was also analyzed to see whether it might predict cognition. The brain’s outer layer, called gray matter, typically contains a high volume of neurons. The decreased quantity of gray matter predicted lower test results in two of the five cognitive domains. This result suggests that monitoring the depletion of synapses may more accurately depict the brain changes affecting cognitive performance.
Due to the in-depth nature and findings of the study, medical professionals can now track the depletion of synapses in dementia patients and comprehend the patient’s cognitive deterioration thanks to imaging data. As a consequence, the imaging findings can help researchers better understand the neurobiology of the condition and assess the effectiveness of Alzheimer’s medications.